My thoughts on the background of the EpiPen mess and how to solve it, today in Jacobin.
Jacobin: “Obama on Obamacare”
Obama recently penned an assessment of the Affordable Care Act in JAMA; I wrote a response in Jacobin.
Chest: “Should Pulmonary/ICU Physicians Support Single-payer Health-care Reform? Yes”
I co-write an editorial with Phil Verhoef and Jesse Hall in which we make the case that intensivists and pulmonologists should support single payer. It’s available (for now) here: http://authors.elsevier.com/a/1TKr62p-km2aS. It’s paired with a counterpoint by Gilbert Berdine, and rebuttals from both sides.
The New Republic: “The Dawn of Antidepressants”
I have a review in the New Republic on Peter Kramer’s new book Ordinarily Well, on the essential question of whether antidepressants indeed work.
Blog Post: What’s Wrong with Margot Sanger-Katz’s Single Payer Analysis
Yesterday, New York Times health care reporter Margot Sanger-Katz, whose work I very much respect, entered the debate on the costs of Sanders’ single payer plan in a piece I find problematic, headlined “A Single-Payer Plan From Bernie Sanders Would Probably Still Be Expensive.” I should first concede, however, the central argument of her article: it is true that a US single payer system would still be relatively expensive as compared to other single payer systems. We would, that is to say, continue to spend more than the United Kingdom or Canada if we transitioned to single payer. At the same time, there would nonetheless be enormous savings from such a transition, and these savings would allow us to affordably achieve real universal health care. This, in my opinion, would still be an excellent deal.
The background to this debate are two analyses of the Sanders’ single payer proposal—the first by economist Kenneth Thorpe and the second by the Urban Institute—both of which claimed that the actual costs of Sanders’ single payer plan would be significantly higher than what his campaign has predicted. The assumptions of each have been convincingly contested by colleagues David Himmelstein and Steffie Woolhandler: among other points, they argue that both analyses underestimate administrative savings and overestimate the cost of increased health care use resulting from a coverage expansion.
Anyway, without delving into the details, there is something rather puzzling when looking at the analyses of Thorpe and the Urban Institute from a broader perspective. How is it that single payer would massively increase costs in the United States, as these reports contend, even while countries with single payer-type systems—like Canada and the United Kingdom—have much, much lower health care costs than we do?
To answer, a quick side note: our total health spending is, by definition, equal to the quantity of health services delivered multiplied by their price. The US does not consistently use more health services than other high-income nations. Therefore, the fact that we have higher health care costs is mostly explained by higher unit prices for services, as Sanger-Katz and others note. Now us single payer advocates cite lower administrative costs (and lower drug spending) as the major sources of savings under US single payer (effectively lowering the “price” side of the equation). But Sanger-Katz argues that this would be insufficient: prices would have to be slashed across the board, and some services would have to be cut:
Making the American health care system significantly cheaper would mean more than just cutting the insurance companies out of the game and reducing the high administrative costs of the American system. It would also require paying doctors and nurses substantially lower salaries, using fewer new and high-tech treatments, and probably eliminating some of the perks of American hospital stays, like private patient rooms.
Such a transition would, she notes, have some scary sounding downstream consequences: “…making big cuts all at once to doctors and hospitals could cause substantial disruptions in care. Some hospitals would go out of business. Some doctors would default on their mortgages and student loans.” My understanding is that we aren’t really allowed to effectively default on student loans, but admittedly this all sounds rather dicey.
But this frightful health care meltdown isn’t even in the cards. She is correct in a narrow sense: it’s true that immediately lowering US health care expenditures to, say, that of the United Kingdom — i.e. from 16.4% to 8.5% of gross domestic product — would require major, disruptive reductions in spending across the board. However, nobody is contending that we do that. The central claim for US single payer is more modest. Use the enormous administrative savings generated under single payer financing in combination with pharmaceutical savings to cover everybody with comprehensive benefits and no cost-sharing. Overall national health spending would, it is true, remain roughly the same (though we could better control cost growth moving forward). But this scenario of widespread hospital bankruptcies and the end of private (or semiprivate?) hospital rooms is a fantasy: nobody wants it to happen, and it’s not happening.
It’s worth noting that there is also a jarringly inconsistent aspect to single-payer critiques that warn of the threat to health care workers’ income. As Woolhandler and Himmelstein note in an article in the Huffington Post, the Urban Institute simultaneously asserted that the coverage expansion under single payer would lead to an enormous increase in spending on physician services — by $1.6 trillion over a decade!—while simultaneously asserting that physician salaries would be “squeezed.” Whatever one thinks of how much physicians should be paid, it’s hard how these would both happen at the same time.
Transitioning to single payer will not mean reducing our health care expenses to British levels: that is probably not possible, and is certainly not desirable. But that’s not to say that the savings from adopting a single payer financing system wouldn’t be substantial—we’re talking hundreds of billions annually on administrative savings alone, plus more by reducing drug prices to European levels. With that money, we’ll build a much more decent health care system for all to use without having to worry about the cost of being sick, of being pregnant, or simply of obtaining preventive care. No wonder a majority of the country wants it.
Physicians’ Proposal for Single Payer
Yesterday was an important day for the single payer movement. We launched the “Physicians’ Proposal for Single-Payer Health Care Reform” at a 1 PM press conference at the National Press Club in Washington. Dr. Robert Zarr, president of Physicians for a National Health Program (PNHP), presided. Participants (from left to right in this photo tweeted by AMSA President Kelly Thibert) included co-founder of Public Citizen’s Health Research Group Dr. Sidney Wolfe, National Nurses United Co-President Karen Higgins, Dr. Claudia Fegan, Dr. Zarr, myself, and Dr. Steffie Woolhandler:
Everybody in, nobody out! #SinglePayer #HCFA @AMSANational @PNHP pic.twitter.com/zatk4WtF5e
— Kelly Thibert (@KTOTUS) May 5, 2016
The Physicians Proposal is a detailed blueprint for a single payer system, as well as a comprehensive critique of the shortcomings of our current system. It was formulated by a 39 member working group, co-chaired by Dr. Marcia Angell, Dr. David Himmelstein, Dr. Steffie Woolhandler, and myself. It was published yesterday alongside an editorial we wrote in the American Journal of Public Health. The proposal is available here (and is open for more endorsements), and the AJPH editorial is open-access and available here.
The release has gotten some good coverage so far, including in:
US News & World Report (“Doctor Group Pushes for ‘Single-Payer’ Model”)
The Guardian (“‘We need fundamental changes’: US doctors call for universal healthcare”)
The Washington Post (“2,000 doctors say Bernie Sanders has the right approach to health care”)
The Hill (“More than 2,000 doctors join call for single-payer healthcare”)
Morning Consult (“More Than 2,000 Doctors Back National Single-Payer Proposal”)
I also had the opportunity to discuss single payer on Thom Hartmann’s show “The Big Picture,” which aired at 7 PM last night:
The fight for universal health care in America continues.
Jacobin: “Saving the NHS”
I had an article in Jacobin today on the ongoing Junior Doctors strike in England, and its larger political meaning.
The New Republic: “Google Knows Your Sick”
I have a review up today of Elad Yom-Tov’s interesting new book, Crowdsourced Health: How What You Do On the Internet Will Improve Medicine.
Blog Post, St. Patrick’s Day Edition: What’s going on with universal health care in Ireland?
In recent years, several nations have announced bold plans for sweeping universal health care reform. One of these is India, which, as it has turned out, has done basically nothing to achieve that goal under the BJP government of Narendra Modi. However, as today is St. Patrick’s Day, I’ll discuss the case of Ireland, which hasn’t made much progress either.
A recent article in the journal Health Policy (“From universal health insurance to universal healthcare? The shifting health policy landscape in Ireland since the economic crisis”) by Sara Ann Burke and colleagues at the Centre for Health Policy and Management at the Trinity College of Dublin School of Medicine explains this well. It’s very much worth reading (and is open access!). It traces the trajectory of “universal health care” reform in Ireland over the past 5 years. In what follows, I’ll summarize some of the main points of that article (interspersed with my own commentary) to give a sense of the health care scene in Ireland.
In 2008, Wall Street sunk and, as we all know, took the global economy down with it in the process. Recession brought about the era of austerity in Europe, and this had the effect of starving health care systems throughout the continent. Ireland was one of the nations facing fiscal and health system austerity. Nonetheless, as Burke et al. note, the 2011 election in Ireland put a new coalition government into power that declared the goal of achieving universal health care. Why was this necessary? Don’t all high-income nations except the US already have “universal health care”? Well, not exactly.
Ireland, for instance, has long had a “two-tier” public-private health care system, as Burke et al. describe. A public system, they note, which goes by the name of the “General Medical Services” (GMS) scheme, covers a substantial minority of the population: these low-income individuals get free GP services as well as low cost prescription medications (those without GMS coverage, on the other hand, have to pay more than €50 for a primary care visit). However, as they emphasize, almost half of the population is covered through private health insurance, a benefit that gives them superior access to hospital care.1
Now, as they note, the government’s 2011 plan for universal health care called for a level playing field, which sounds like a step in the right direction. However, this wouldn’t be through single payer transformation, but instead through a Dutch-style reform, with everybody mandated to purchase a plan from a for-profit private health insurance company.2
However, the Dutch approach has serious shortcoming, as I recently wrote about in Jacobin. I noted the following, in describing some of the parallels between the Dutch reform and the Affordable Care Act:
If the Netherlands model demonstrates anything, it’s that some forms of “universal” health care are less worthy of emulation than others. Expanding access the Dutch way (itself based on US policy ideas) would leave intact much of the waste of the current system — without achieving the equity implied by the term ‘universal health care.’
To be fair, as Burke et al. describe, the Irish government was also proposing that everybody would at least get free GP visits under the reform, which would no doubt be a significant and meaningful improvement. Regardless, basically none of this came to pass. As they describe, the last five years have seen no major change in health insurance coverage in Ireland: the percentage of the population with GMS cards saw no major change, while some evidence pointed to a rise in wait times. At the same time, they state, the government retreated from its previous calls for “universal health care” and free GP visits for all (it did expand free GP visits to those > 70 and those < 6, though that was about it).3
They thus conclude:
While there has been an intent of universalism in official government policy since 2011, the data presented here show little progress made on increasing the breadth, with decreasing depth and scope of coverage of coverage evident through increased user charges and numbers waiting for hospital diagnosis and treatment. The exception is the extension of free GP care to the youngest and oldest citizens in mid-2015 and a small increase in private health insurance in 2014/5. This failure to progress towards universalism can be explained by the unrelenting pressure on the health system as a result of budget cuts since 2009 and by the lack of clarity on the exact form of universalism espoused and the mechanisms to achieve it.4
This paragraph lays out the problem very succinctly. On the one hand, the system was hard pressed by the financial demands of austerity. Others have emphasized the effect of austerity on health care in Ireland: at a time when people needed more protection, not less, coverage fell while copayments (“user fees”) rose. Here is Alexander Kentikelenis, for instance, in the European Journal of Public Health:
Ireland also implemented steep health sector cuts in 2012 as part of the fiscal adjustment programme agreed on with its international creditors, and introduced a rise in user fees. The onset of austerity marked a reversal in the extent of coverage, and tightened eligibility criteria for issuing [GMS] ‘medical cards’—a means-tested programme for the poor—resulted in the decline of people covered under this programme.5
And on the other hand, Burke et al. note that the “exact form of universalism” being pursued was unclear, which is exactly right: unlike a comprehensive national health insurance or national health system reform, the government, they suggest, envisioned a system run by private insurers as in the Netherlands or, to an extent, in the US.
However, even that reform didn’t come about. Ireland, like the US, as a result still lacks true universal health care, with equitable access to all. Looking ahead, Burke et al. write,
Ireland is at a critical juncture, veering between a potential path to universal healthcare and a system overwhelmed by seven years of austerity, which continues to maintain the status quo and a historical bias towards a two-tier unequal system of care.6
Unfortunately, people in nations throughout the globe are contending with similar problems: inadequate funding and unequal health system access. But private health insurance – whether dubbed “universal” or not – is not the answer, either for Ireland or the US.
Notes
1 Burke SA, Normand C, Barry S, Thomas S. From universal health insurance to universal healthcare? The shifting health policy landscape in Ireland since the economic crisis. Health policy 2015. In press.
2 Ibid.
3 Ibid.
4 Ibid.
5 Kentikelenis A. Bailouts, austerity and the erosion of health coverage in Southern Europe and Ireland. European journal of public health 2015;25:365-6.
6 Burke SA, Normand C, Barry S, Thomas S. From universal health insurance to universal healthcare? The shifting health policy landscape in Ireland since the economic crisis. Health policy 2015. In press.
The New Republic: “How Liberals Tried to Kill the Dream of Single-Payer”
I have an article online today at The New Republic where I take on both the political and economic arguments being hurled at single-payer.
LA Review of Books: “Is the Path to Racial Health Equity Paved with ‘Reparations’? The Politics of Health, Part II”
I have a review/essay in the Los Angeles Review of Books today. It’s the second part of the “Politics of Health.” The first part mainly dealt with health inequalities by class, whereas this part deals with health inequalities by race. I review two recent books: Dayna Bowen Matthew’s Just Medicine: A Cure for Racial Inequality in American Medicine and Damon Tweedy’s Black Man in a White Coat.
#SuperTuesday
Ballot cast. Let the games begin.

560+ Physicians and Medical Students Agree: Time to Move on Medicare-for-All
More than 560 doctors and med students have signed onto an open letter organized by the Ad Hoc Committee on Medicare-for-All, now published at The Huffington Post:
The renewed debate over the merits of single-payer health reform has been marred by misleading claims that such reform is unnecessary and unaffordable. We write to set the record straight…
It’s not too late to join us: follow this link to add your signature and help turn the tide.
Time to Set the Record Straight on Single Payer
Recent weeks have seen a slew of misleading attacks on the affordability and merit of single payer health care. It’s time to set the record straight.
Please see “Setting the Record Straight on Medicare-for-All: An Open Letter From Physicians and Medical Students.” The letter went up today. You can endorse the letter on the webpage. A list of endorsers will be published in the near future. Please also circulate to colleagues. This is a crucial moment in the national debate over health care reform and single payer.
Blog: Contraception Coverage and the ACA
A “viewpoint” article published in JAMA this week (authored by March C. Politi, Adam Sonfield, and Tessa Madden) briefly summarizes how the Affordable Act Act (ACA) expands access to contraception, but also describes the various “challenges” that thus far have prevented the full implementation of this provision.
To my mind, the points they make demonstrate how the underlying, structural flaws of our health care system make even relatively straightforward and useful reforms like the ACA’s contraception mandate enormously difficult and complex to realize in practice.
As they briefly summarize in the article (“Addressing Challenges to Implementation of the Contraceptive Coverage Guarantee of the Affordable Care Act”), the ACA includes a provision that mandated that contraception-related health care - including medications, devices, services (including sterilization), office visits, and education - be covered by privates insurers without “cost sharing” (i.e. copayments or deductibles).
This is unquestionably a good and useful measure: contraception-related care is a fundamental component of comprehensive reproductive health care. There is no plausible reason to punish women who use contraception by imposing out-of-pocket payments at the time of use (the same could be said of all medically-necessary health care, in my opinion, but that’s a story for another time).
The article then briefly summarizes the various games insurers have played in preventing the implementation of this rather straightforward provision. For instance, they note that some insurers have left out coverage for certain modes of contraception (though they assert that this should be addressed by new federal rules), and also that insurers have not been reliably covering contraception-related clinical care. “Inappropriate insurance practices,” they write, “may therefore lead to patients being erroneously charged for services that should be covered with no out-of-pocket costs, potentially interfering with patients’ ability to practice contraception consistently and effectively.”
But it is when they turn to the issue of billing and coding that the ridiculous complexity of our health care system - and the harm that this complexity causes - becomes most evident. As a result of the vagaries of billing codes, what is theoretically fully covered may not be in practice. As they write:
Physicians, other clinicians, and health care organizations may find it difficult to appropriately bill for contraceptive services in a way that ensures that patients are properly exempt from cost sharing. If a patient receives contraceptive counseling as part of a well-woman examination, the situation is straightforward because the well-woman examination has a specific Current Procedural Terminology code and is considered a covered preventive service. However, if a patient has an office visit solely for contraceptive counseling (which does not have a specific billing code), the clinician or health care center must bill an appropriate evaluation and management code (which can be used for many purposes) and billing modifier (ie, 33) to specify that the visit was for the preventive service, contraceptive counseling. Many clinicians and health organizations are unaware of this modifier, and some insurers have been slow to program their billing systems so that this modifier automatically triggers the patient’s exemption from cost sharing when the included diagnosis codes (formerly International Classification of Diseases, Ninth Revision [ICD-9], now ICD-10) indicate that primarily preventive services were provided.
Of course, it is ultimately women who are penalized by this byzantine structure of coding.
But the complexities don’t end there. As they describe:
An additional challenge arises if care that involves diagnostic testing is provided during a visit, even when the initial visit was scheduled for contraceptive counseling or maintenance. Under the ACA provision, a visit should be considered preventive—and therefore exempt from cost sharing—if the primary purpose of the visit is for preventive care. However, the primary purpose may not always be clear to patients, clinicians, and payers when additional care is provided. Clinicians can use 2 separate billing codes, one for the preventive care and an additional code for the diagnostic care, but this could lead to confusion and disagreement about when patients will be charged. Greater transparency could help clinicians and health care centers communicate with patients about these potential fees.
This is of course ridiculous. In reality, office visits can be a combination of things, and attempts to classify them as purely “preventive” or not is a fiction. It’s also entirely unnecessary: if office visits for both “preventive” care and “non-preventive” both didn’t have cost sharing, none of this would matter (at least from the patient’s perspective).
They finally note that none of these protections are available for women who obtain contraception-related services “out-of-network.” Yet this may happen unwillingly: as they describe, a women may undergo a sterilization procedure at a facility that’s inside of the insurance network, but the anesthesiologist involved in the case may be out-of-network.
The story of the contraception coverage mandate of the ACA thereby speaks to the enormous difficulty of effectively - much less efficiently! - moving towards universal health care within a structure dominated by private insurers.
Blog: What Does the Medicare Rollout Say About Single Payer?

An interesting article today in Huffington Post by Steffie Woolhandler and David Himmelstein - both health policy scholars and co-founders of Physicians for a National Program - looks back at the history of Medicare for lessons about single payer today.
They make a few notable points in the piece, which is headlined “Medicare’s History Belies Claim That Medicare-for-All Would Disrupt Care.” First, they note that the implementation of Medicare was actually quite smooth. As they describe, cards were sent to the homes of all the elderly, and those who lived in more remote locations were contacted through various outreach programs; predicted doctors’ strikes never happened, and the health system wasn’t overloaded by the demands of new beneficiaries. Moreover, the process was relatively efficient: by their calculations, the rollout of the Obamacare “marketplaces” cost some seven times as much as the (inflation-adjusted) rollout of Medicare.
Second, they note that Medicare was “disruptive” in a good way: it helped undo the reign of Jim Crow medicine. As they note, the implementation of Medicare forced the segregation of Southern hospitals. At the same time, however, they rightly emphasize that de facto segregation continues today when patients with different insurance plans are treated separately. In contrast, “Medicare-for-All,” they write, “would give all Americans complete and equal coverage, completing the disruption of hospital segregation that Medicare began a half century ago.”
There is a broader point here, about the role of a true universal health care - without tiers and without financial barriers to care - in the fight against racial health inequalities. Despite all the research and discussion around the issue of “health disparities,” this issue gets insufficient attention. I discuss it in a lengthy review/essay about racial health inequality which will be published in the Los Angeles Review of Books sometime in the coming weeks.
Blog: Latest Results from the National Health Interview Survey
Uninsurance remains a problem in America, even in the age of the Affordable Care Act (ACA). That’s one conclusion that can be drawn from the latest survey results released two weeks ago by the National Center for Health Statistics.
The report (“Early Release of Estimates From the National Health Interview Survey, January–September 2015”) compares survey data on health insurance coverage gathered over the first nine months of 2015 with that of previous years, extending back to 2010. The estimates rely on a civilian, non-institutionalized sample, which for 2015 consisted of some 79,847 individuals in 37 states. I’ll briefly summarize some of the key results in this post.1
The survey demonstrates a substantial reduction in the uninsured population in the years following the implementation of the ACA. In 2010, 22.3% of non-elderly adults were uninsured at the time at which they were interviewed. In contrast, for the first 9 months of 2015, this had fallen to 12.9%. This comes after about a decade of rising uninsurance, beginning in the late 1990s:
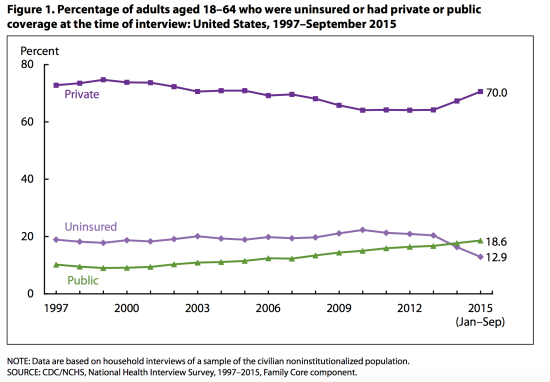
The time trends by age groups are as one might expect. For younger adults (ages 18-24), the reduction in uninsurance occurred over 2010 and 2011. This makes sense, as the dependent coverage provision of the ACA was implemented in September 2010 (the law required coverage of children below age 26 under family health insurance plans). For other age groups, in contrast, uninsurance fell between the years 2013 and 2015. This squares with the fact that the main coverage expansion provisions of the ACA – i.e. the individual mandate and the Medicaid expansion – went into effect in 2014.
Inequalities in insurance status by class persist. In 2015, among non-elderly adults, 26.1% of the poor and 24.1% of the near-poor were uninsured at the time the interview was conducted, as compared to 7.7% of those who weren’t poor. However, there were notable reductions in uninsurance among the former two groups between 2013 and 2015:
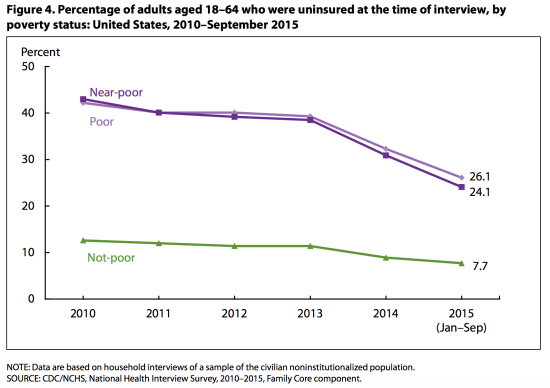
Coverage inequalities by race – despite improvements – also persist. In 2015, among non-elderly adults, 27.9% of Hispanics and 14.6% of non-Hispanic blacks were uninsured, as compared with 8.8% of non-Hispanic whites and 7.3% of Asians:
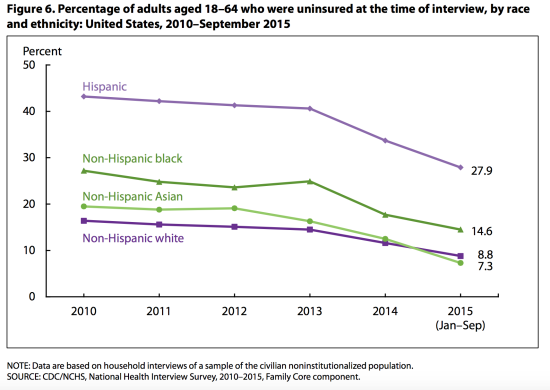
Addressing racial health inequalities, clearly, requires addressing these inequities in coverage (among many other things).
There were also inequalities by geography. Unsurprisingly, uninsurance among non-elderly adults was higher in states that have not yet expanded Medicaid under the ACA as compared to those that have (see this analysis for estimates of the number of deaths that have needlessly resulted from this “opt out”).
Finally, the survey reveals the evolving character of insurance: high-deductible heath insurance plans are on the rise. The percentage of the privately insured non-elderly with high-deductible health care plans (whether or not they are associated with a health savings account) rose from 25.3% in 2010 to 36.2% in 2015:
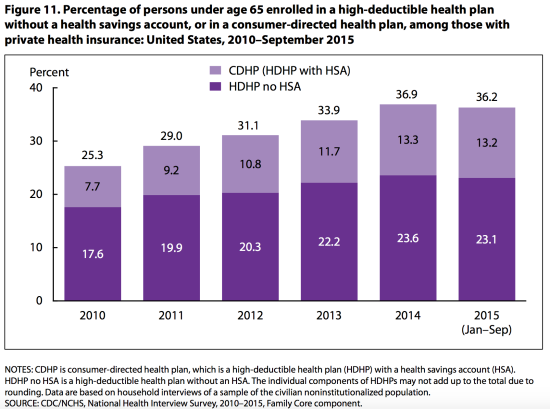
This is but one glimpse at a much larger story of rising deductibles and copayments – of underinurance more broadly – in the United States.
In sum, the ACA has clearly expanded coverage in the United States. In 2010, among those of all ages, 48.6 million were uninsured (determined based on the time they were interviewed) according to the estimates of this survey. For the first nine months of 2015, this had fallen to 28.8 million. This is no doubt a meaningfully and important change for the many millions who are now newly insured. Yet, the law is now in full effect, and millions are still excluded from coverage. Moreover, inequalities in coverage – along the lines of both race and class – persist. High-deductible health plans are on the rise. Universal health care has not yet been achieved.
————-
1 Note that all the figures reproduced here from the report are in the public domain. All numbers cited in this post are from this survey. When I say “2015,” I am referring to the first nine months of 2015. “Non-elderly adults” describes those aged 18-64.
Newsletter #2: The Single Payer Debate Continues
For now, I’ll keep posting my (brief) newsletters here. Apologies for those who come across it twice! You can signup for the newsletter here if interested: http://tinyletter.com/awgaffney
———————
Dear PP Subscribers,
The Democratic primary race has intensified. Contests in Nevada and South Carolina are looming. The debate over single payer remains fierce.
The last few weeks have seen continued arguments from a spectrum of commentators as to why a Medicare-for-all program – like that proposed by the Sanders campaign – is untenable.
A number of overlapping lines of argument can be distinguished. First, it is frequently argued that the Sanders plan is poorly formulated and/or unrealistic given political conditions in Washington. Recently, for instance, Paul Starr in the American Prospect (headlined “The False Lure of the Sanders Single-Payer Plan”) argues that the Sanders proposal is “not a practical or carefully thought-out proposal.” Indeed, he sees the plan as an indictment of his overall campaign: it’s “a symbolic gesture, representative of the kind of socialism he supports.”
I addressed some of the earlier (and similar) liberal criticisms in an article published January 21 in US News & World Report, “Single Payer is Worth Fighting For.” I conclude:
The expansion of coverage achieved by the Affordable Care Act does not constitute a system of universal health care. Too many are uninsured and underinsured. Too many are squeezed by high deductibles, contend with “narrow networks” of doctors and hospitals, or face crushing medical bills and even bankruptcy. Single-payer is the best way to remedy these injustices while simultaneously controlling overall health spending.
I also chatted about some of these issues on the radio with Arnie Arnesan on WNHN 94.7, available here.
A second line is that single payer is simply not affordable - that the number don’t add up. For instance, in casting doubt on the seriousness of the Sanders’ single payer proposal, Starr relies on the widely-covered estimates of Kenneth Thorpe, an economist at Emory University. Vox covered Thorpe’s new estimates, which put the price of Sanders’ single payer proposal at nearly twice what his campaign has contended.
However, David Himmelstein and Steffie Woolhandler have clearly demonstrated the flawed assumptions behind these numbers in this detailed post at the Huffington Post, which is well worth reading. As they put it:
Thorpe’s analysis rests on several incorrect, and occasionally outlandish, assumptions. Moreover, it is at odds with analyses of the costs of single-payer programs that he produced in the past, which projected large savings from such reform […] In the past, Thorpe estimated that single-payer reform would lower health spending while covering all of the uninsured and upgrading coverage for the tens of millions who are currently underinsured. The facts on which those conclusions were based have not changed.
A third line admits the shortcomings of the current state of affairs in American health care, but suggests that the right way forward would be to expand towards universal coverage under the ACA – instead of pursuing the more fundamental change of single payer. I address this argument in an article published online Thursday in Jacobin, headlined “What Obamacare Can’t Do.” I turn to a country that has attempted to work towards “universal” coverage through a system of competing private insurers – the Netherlands – to demonstrate why this approach falls short, both from the perspective of cost and efficiency as well as that of equity.Regardless of the outcome of the primary, the campaign for single payer debate is far from over. The incremental reforms have already been accomplished – we now either move backwards or we move ahead.
Until the next sporadically timed newsletter,
Adam
Blog: Implications of a Tight Race
The Democratic primary race has grown tighter and spicier than virtually anyone had predicted. A quick glance at February:
Looking back:
February 1: Hillary Clinton bests Bernie Sanders in the Iowa caucus, but only by the narrowest of victories.
February 5: A national poll puts Clinton and Sanders in a dead heat: as Politico reported, Sanders is at 42% compared with Clinton at 44%. These percentages fall within the margin of error.
February 9: Sanders dominates the New Hampshire primary by a margin of more than 20 points. But perhaps just as important, as David R. Jones noted in a post in The New York Times, Sanders won in essentially all categories of voters:
He carried majorities of both men and women. He won among those with and without college degrees. He won among gun owners and non-gun owners. He beat Mrs. Clinton among previous primary voters and those participating for the first time. And he ran ahead among both moderates and liberals.
February 12: As the Hill reports, another poll demonstrates a tight race, with Clinton having only a 7-point lead over Sanders nationwide.
Looking forward:
February 20: The next Democratic contest, the Nevada caucus. Recent reliable polls seem to be in short supply. For what it’s worth, FiveThirtyEight’s “polls-plus” analysis gives the two candidates an equal chance of winning. On Friday, Slate’s Jim Newell described Clinton’s numerous advantages in the state – her so-called “Western firewall” – but also notes that “it wouldn’t be surprising if this firewall is crumbling, or whatever it is that firewalls do when they stop being firewalls.” Do they smolder, or are they quenched?
February 27: The South Carolina primary. This is seen as Clinton’s real “firewall,” as the odd saying goes. According to FiveThirtyEight, she is set to dominate the state. However, a long report, well worth reading, by Joyn-Ann Reid at MSNBC headlined “Warning signs for Hillary Clinton in South Carolina” argues that the situation in that state may be less settled than polls may suggest.
Time will tell. In the meanwhile, the tightening of the race has meant that single payer health care has remained front and center of the national political discussion. For single payer advocates it is a crucial time to continue pressing the cause.
Jacobin: “What Obamacare Can’t Do”
Today in Jacobin, I write about why single payer remains critical to the goal of universal health in the US - and why other roads will fail.